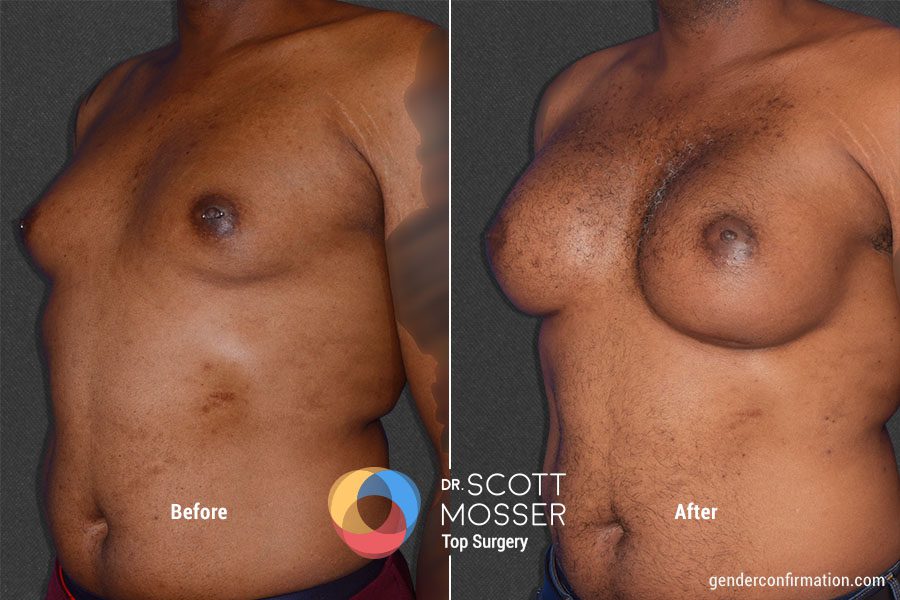
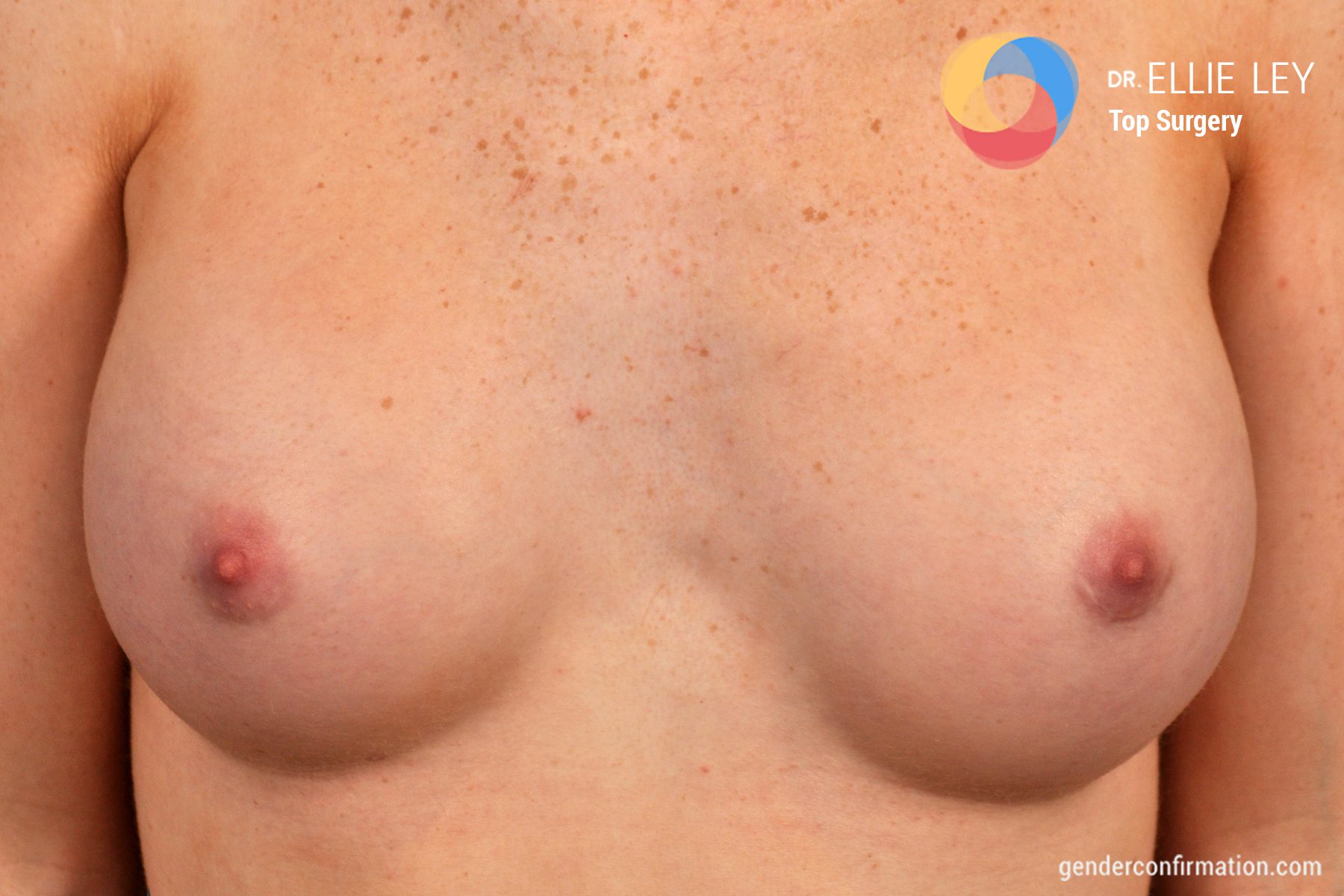
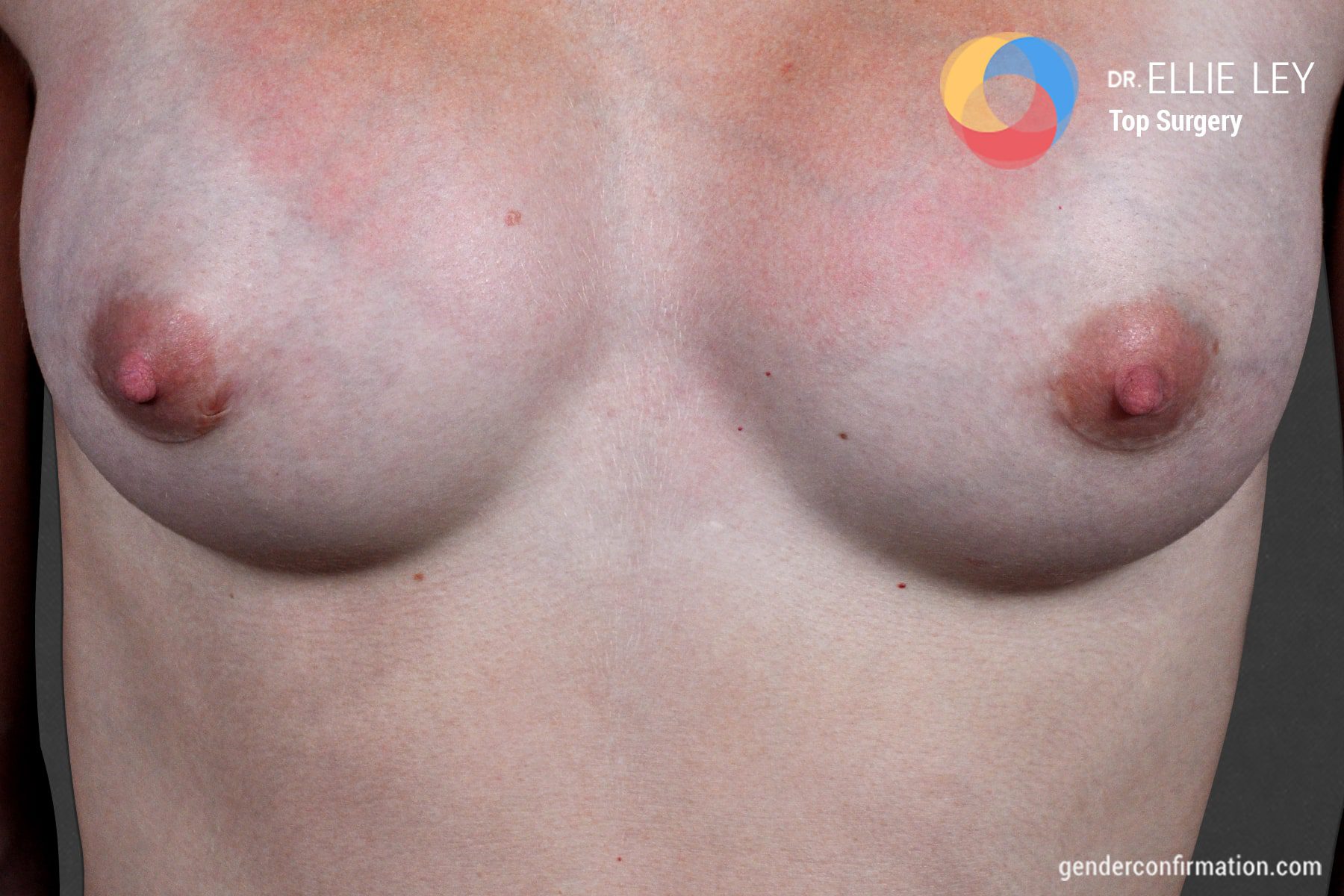
MTF Breast Augmentation for Gender-Affirmation
Medically reviewed by Brianna Smith on April 29, 2026.
Finally, a group of expert top surgeons inclusive of all identities and body types, with a highly successful insurance concierge.
Transgender breast augmentation, also known as MTF top surgery, is a surgical procedure that increases the volume of the breasts with implants and/or fat grafting. Even with hormone replacement therapy (HRT), trans women and trans-feminine non-binary patients tend to have anatomical differences compared to cis women that should be taken into account for the design of their surgical plan. Patients that are on estrogen HRT are often advised to wait 1.5-2 years to develop their breast tissue before undergoing surgery. You can request a free virtual or in-person consultation with one of our board-certified surgeons in San Francisco or Pasadena if you are interested in undergoing gender-affirming surgery.
On This Page
What is a Gender-Affirming Breast Augmentation?
How Can I Get Feminizing Top Surgery?
Our Board-Certified Breast Augmentation Surgeons:
To perform a gender-affirming breast augmentation, your surgeon can choose from a variety of techniques to enlarge or construct breasts: principally through implants or liposuction-fat grafting. Transgender and non-binary patients often have different needs than cisgender women seeking breast augmentations. For example, wider breast implants and specific placement techniques may be necessary to help a trans patient meet their goals due to common anatomical factors (e.g., a wider sternum and rib cage, more space between nipples, etc.). For this reason, we encourage patients to consider board-certified surgeons who are specialized in working with trans patients.
Surgery for Trans and Non-Binary Patients at the GCC
At the Gender Confirmation Center (GCC), we have performed over 5,000 gender affirming procedures since 2009 using state-of-the art medical technology. In an effort to make the safest, highest quality surgical care financially feasible, our insurance concierge service has successfully secured insurance coverage for 90% of interested patients. At the GCC, we are unique in our commitment to making gender-affirming surgeries accessible to patients of all gender identities, regardless of hormone usage, body mass index (BMI), age or disability.
If you are interested in surgery, you can request a free, virtual or in-person consultation with us today. If you have already undergone surgery and have questions about recovery, complications or revision surgeries, you can click on the hyperlinked articles.
Transgender Breast Augmentation Techniques and Options
When it comes to feminizing top surgery, patients can personalize their procedure when it comes to the following factors we discuss below: implant type, implant shape, implant size, incision location, and implant placement. Our surgeons can help you navigate these choices based on your unique anatomy and goals in a free consultation.
Augmentation type: fat grafting vs. saline & silicone implants
The fat grafting technique is less common amongst transfeminine patients because of its low success rate when a large amount of volume is needed and the skin is particularly tight. This means that the first choice for most patients is between silicone and saline implants. Fat grafting can be used in addition to implants, for example, to increase medial cleavage between the breasts.
Silicone implants have become the most popular choice amongst our patients because of their durability, softer feel and appearance, especially for those starting out without a lot of breast tissue.
Implant Shape
A patient can also choose the shape of their implants. Specialists in transgender care know that trans patients will often need wider implants than their cis counterparts to meet their goals.
At the GCC, we prefer round or circular to teardrop-shaped implants for a number of reasons. First, if your implants rotate, round implants will not pose a risk to breast symmetry. Second, circular implants allow for more options around placement and a smaller incision for insertion, which reduces the size of the scar. Third, once patients results have healed, the difference between tear-drop shaped and round breast implants on breast contour is practically imperceptible, especially for implants placed below the muscle.
Breast or Implant Size
Rather than measuring by cup or bra size, the size of breasts are determined by the implant size, which typically ranges from 200cc-500cc. The final appearance of your breast size will have a lot to do with your unique anatomy. We encourage patients to try out the rice bag test at home to figure out which size would best suit your needs. Likewise, during an in-person consultation we allow patients to try on implant sizers.
MTF Top Surgery Scars & Incision Type
Your surgical scars are determined by the incision location, i.e., where the breast implant will be inserted. Patients main concerns tend to be about minimizing scar visibility and creating an incision that allows for optimal implant placement. For these reasons, we most commonly make an incision along the inframammary fold, which conceals the scar at the fold at the bottom of the breast. Scar texture and discoloration can often be reduced with proper care.
Patients can also opt for an incision along the border of the areola (periareolar) or through the armpit (transaxillary). Most transgender patients we see do not have large enough areolas to insert a silicone implant. Although the scar is hidden, inserting implants through the armpits is associated with higher rates of capsular contraction, bleeding and placement complications, which is why we no longer offer this option at the GCC.
Implant Placement
Placement refers to the option to place the implants below the muscle (submuscular) or above the muscle and below the mammary glands (subglandular). Some surgeons who offer a submuscular placement will offer to score the pectoral muscles to help the implants settle.
Surgeons can also perform a dual plane technique (placing the implant partially under & partially over the pectoral muscle) or a subfascial technique (placing the implant below the fascia). You can read more about the advantages and disadvantages of each technique here.
Implant Texture
Due to increased risk of breast cancer associated with textured implants, the GCC only offers smooth implants to our patients,
How Can I Get Feminizing Top Surgery?
There is a lot that goes into preparing for top surgery, which can make it confusing and even overwhelming for some. The information below is meant to help guide you on the steps that most patients go through in order to schedule their surgery date. Afterwards, there are steps you will need to take to prepare yourself for surgery.
What are the steps involved to undergo MTF top surgery?
The first step in a patient’s journey is requesting a free consultation. From there, we have you covered with our feminizing top surgery timeline guide.
Will my insurance cover transgender breast augmentation?
Some insurance providers do cover gender-affirming surgeries as medically necessary procedures. For those that do, requirements often include:
- Patient must have been on at least 12 months of continuous feminizing HRT, unless there is a medical contraindication
- Patient must present a support letter from a licensed mental health provider
At the GCC, you can leave the insurance worries to us. We provide a free insurance concierge service to interested patients. After soliciting any necessary documents from you, our insurance advocacy team will get to work to secure full or partial coverage for your medically necessary, gender affirming procedure(s). Our team has a 90% success rate in securing coverage for insured patients. Learn more about those services here.
How can I finance my surgery if it’s not covered by insurance?
We have compiled a list of grants for gender affirming surgeries alongside trusted, medical credit agencies you can use to help finance your surgery with us. On the same page, you can also find estimated costs for each procedure we offer if you plan on paying entirely out of pocket.
How long should I be on HRT before getting a breast augmentation?
Generally, patients who are taking feminizing HRT are recommended to let their breast tissue develop for 1.5-2 years under treatment. Patients who microdose estrogen may be advised to wait longer to maximize mammary tissue growth and, in turn, breast augmentation results. That said, we have no HRT requirements to undergo this surgery. That said, we have had successful results with patients who come in with no initial mammary tissue. There are several non-binary patients that have undergone breast augmentation surgery with us that have no interest in taking HRT.
What can I do if I need to travel for surgery?
Many trans, non-binary and gender expansive patients need to travel to access quality, reliable gender affirming surgical care. At the GCC, we are very accustomed to working with patients that come in from out of town. For recommendations on travel and lodging, click here. We have also compiled a guide on preoperative consultations and post-operative follow-up protocols for patients who do not live in the San Francisco Bay Area.
What should I do to prepare for MTF breast augmentation?
We have prepared a guide specifically for breast augmentation patients on how they can prepare for surgery in the days leading up to it. Additionally, exercise and drug consumption are two of the most important factors to monitor before your surgery that can help you maximize your results and speed up your healing process. Learn more about our guidelines and recommendations around exercise and drug use here.

Dr. Alexander Facque (he/him)
Dr. Alexander Facque (he/him) is a board-certified plastic surgeon and proud member of the LGBTQ+ community. Dr. Facque got his start in gender-affirming care as a resident at the Icahn School of Medicine at the Mount Sinai Medical Center in New York, where he first recognized the importance of providing safe and accessible surgeries to trans and non-binary patients. He then spent a year training and expanding his knowledge under Dr. Loren Schechter, one of the world’s foremost gender-affirming surgeons, as a fellow at Weiss Memorial Hospital’s Gender Confirmation Surgery and Practice Leadership in Chicago. Dr. Facque officially joined our team in 2020 and brought with him over 5 years of previous experience in gender affirming care.

Dr. Ellie Zara Ley (she/her/they)
Dr. Ellie Zara Ley (she/her/they) is a board-certified plastic surgeon and the only transgender woman of color to offer a full-spectrum specialization in gender affirming surgery: top surgery, bottom surgery, facial surgery and body contouring. She also specializes transgender adolescent care. She is highly trained, having completing her general surgery residency at University of Arizona, a fellowship in plastic and reconstructive surgery at the University of Utah, a fellowships in craniofacial and pediatric plastic surgery at Primary Children’s Hospital in Salt Lake City and another in hand surgery and microsurgery at the University of Southern California. Prior to joining our team in 2022, she worked as an assistant clinical instructor of plastic surgery at the University of Utah and had her own private practice in Arizona.

Dr. Eric Lin (he/him)
Dr. Eric Lin is a board-certified plastic and reconstructive surgeon with nearly 30 years of experience in a variety of breast surgeries. He values the importance of learning about patients’ perspectives to best help them achieve their desired goals. In addition to offering gender surgeries, Dr Lin also remains active as a post-cancer reconstructive surgeon and serves as Clinical Associate Professor of Plastic Surgery at the California Northstate University, College of Medicine.

Dr. Efstathios Karamanos (he/him)
Dr. Efstathios Karamanos is a board-certified plastic and reconstructive surgeon with expertise in microsurgery, breast reconstruction, body contouring, and facial surgery. He has trained at leading institutions in both the United States and Europe and currently serves as Assistant Professor of Surgery at the California University of Science and Medicine. Dr. Karamanos is widely published, serves on multiple editorial boards, and is an active member of national surgical societies.

Dr. Ari Wes (he/him)
Dr. Ari Wes is a plastic and reconstructive surgeon at the Gender Confirmation Center specializing in gender-affirming facial surgery and top surgery. Over the past decade, his training and clinical practice have focused extensively on gender-affirming care, with dedicated experience in facial feminization and chest surgery and a sustained commitment to transgender, nonbinary, and gender-diverse patients. He trained at the Hospital of the University of Pennsylvania and the Perelman School of Medicine, where he developed expertise in craniofacial surgery, breast reconstruction, body contouring, and surgical outcomes research. He is committed to clear communication, thoughtful planning, and meticulous technique so patients feel informed and supported throughout their surgical care.

Dr. Scott Mosser (he/him)
Dr. Scott Mosser (he/him) is a board-certified plastic surgeon who has over 15 years of experience serving gender diverse patients. He has devoted himself exclusively to gender affirming care since founding the GCC in 2013. Dr. Mosser is also a cofounder of the American Society of Gender Surgeons (ASGS), a member of the American Society of Plastic Surgeons (ASPS), the World Professional Association of Transgender Health, (WPATH), the United States Professional Association of Transgender Health (USPATH), and is a Fellow of the American College of Surgeons (FACS).
Recovery from breast augmentation varies depending on the type of procedure you undergo. During the first weeks of recovery, you will need to wear a compression bra for support. Generally speaking, patients that have desk jobs can return to work 1-2 weeks after surgery. That said, you will not be able to return to full physical activity—especially heavy lifting––until 6 weeks after your procedure.
Breast implants are generally placed high on the chest during surgery because gravity will pull them down during the recovery process. Between implants settling and inflammation resolving, patients can expect to see their final results between 6-12 months post-op.
If you have more questions about recovery, you can consult the following guides:
First week of recovery
Returning to exercise
Bruising and swelling
Complications and revision
How much does breast augmentation surgery cost?
After your free consultation, once your individual surgical plan is created, we can provide you with a quote for your surgery. Generally, breast augmentation surgery, including some recovery materials, comes out to $8,500 – $10,000, plus additional costs like facility fees. Insurance coverage can help significantly reduce these costs for patients.
Will the sensation in my breasts and nipples change after top surgery?
All of the breast implant options we offer involve a risk of sensation loss. While most patients report an overall loss in sensitivity of their breasts and nipples post-op, they tend to report higher levels of sexual satisfaction because of feelings of euphoria and alignment with their bodies. We encourage you to ask your surgeon about nerve rehabilitation exercises if you are interested in recuperating sensation.
Can a breast augmentation be performed alongside other procedures like body feminization surgery?
The most common procedure to accompany a breast augmentation is body feminization surgery, which often includes trunk liposuction, BBL, hip augmentation and/or abdominoplasty. In some cases, patients may be able to undergo a small amount of Facial Feminization Surgery (FFS) procedures alongside a breast augmentation. You can speak to a surgeon during a free consultation about your options.
Do implants impact breast cancer risk?
So far, there is little evidence linking saline or silicone breast implants to an increased risk for breast cancer. Otherwise, for patients who have developed breast tissue through hormone replacement therapy (HRT), there is some evidence to suggest that estradiol can increase your breast cancer risk. As a result, it is recommended that if you are over the age of 50 and have been undergoing HRT for 5 or more years, you undergo screening mammography every 2 years.
On the other hand, there is a type of lymphoma that is associated with breast implants. You can read more about risk evaluation and best practices for breast cancer detection in transgender patients here.
Do you have specific questions about top surgery? You can get them answered and start the journey to getting top surgery by requesting a free, virtual consultation with one of our board-certified surgeons.
Click Here to Request the Next Steps to Schedule a Consult!
We offer complimentary virtual and in-person consultations with our board-certified surgeons. Click here to complete our consultation request form to learn more about the next steps in your patient journey.
BOOK CONSULTATION